WOUND ASSESSMENT
 Accurate wound assessment should include a comprehensive patient history, aetiology of the wound, condition of the wound bed and periwound area including the amount, colour, and consistency of exudate as well as signs of infection (Ousey & Atkin, 2013).
Accurate wound assessment should include a comprehensive patient history, aetiology of the wound, condition of the wound bed and periwound area including the amount, colour, and consistency of exudate as well as signs of infection (Ousey & Atkin, 2013).
Patient Assessment
A holistic assessment of the patient is essential to identify the causative or contributory factors and to highlight issues that could delay wound healing. The following factors must be considered when choosing an appropriate plan of care.
General Health Information:
- Medical history
- Age
- Medication and allergies
- Other diseases such as
- Diabetes
- Vascular diseases
- Immune systems that are compromised
- Nutritional status and fluid intake
- Smoking/alcohol
- Obesity
- Mobility
- Continence
- Pressure sore risk
- Oxygen deficit/anaemia
- Skin sensitivity and integrity
- Stress anxiety, sleep disturbances
- Psychological aspects – Impact the wound has on the emotional, physical, and social aspects of the patient’s quality of life
- Mental Health – Feeling good, able to cope
- Emotional Health – Ability to express how they are feeling
- Social Health – Support network
Information provided to patient and/or carers
Recognition of these factors will either delay or promote the wound healing process. Successful wound healing is dependent on the patient’s ability to heal, not the dressing used (Vuolo, 2009).
WOUND ASSESSMENT
 | Accurate wound assessment is vital to give a successful resolution and uncomplicated wound healing. It provides valuable information to enable informed decisions about a patient and their wound. |
|---|---|
WOUND BASELINE INFORMATION
- Number of wounds
- Location – can identify/determine cause and act as an indicator for potential complications
- Cause e.g. trauma, pressure, vascular in insufficiency, neuropathy, other
- Type/classification – e.g. pressure ulcer, skin tears, burns etc
- Duration – date of occurrence, length of time, Acute/Chronic
- Treatment aim – healing, symptom management etc
- Planned reassessment date
It is important that all observations, assessments, planned treatment and interventions of the wound are documented in the patient’s notes. Records must be clear and accurate. It is a helpful way to track the progress of a wound and ensure patients receive continuity of care.
Photography now plays a key role in wound care. The use of digital photography has enhanced the reliability and accuracy of wound documentation. Please refer to your local policy.
WOUND ASSESSMENT
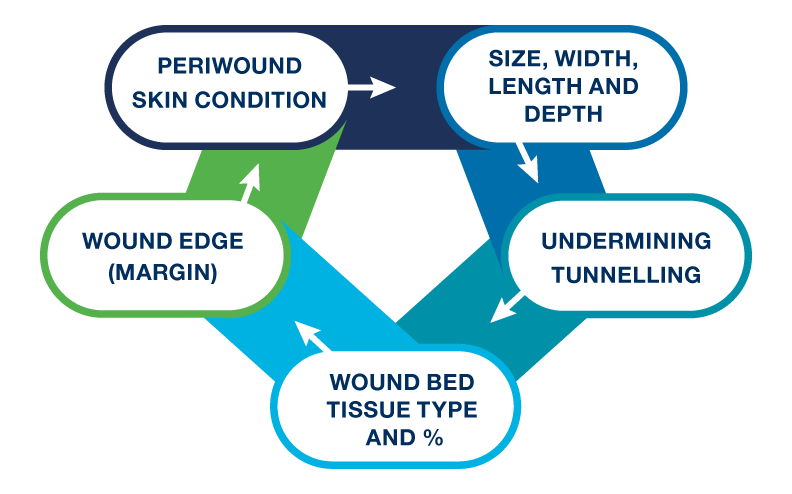
Size, width, length and depth is important to be measured and documented so that the progress of the wound can be measured over time.
Undermining and tunnelling refers to tissue destruction underlying intact skin and along the margins of the wound. Tunnelling course or pathway can extend in any direction from the wound, resulting in dead space.
Wound bed tissue type. A wound can consist of different tissue types, which can be categorized by name and/or colour. Record the percentages of the differing tissue types.
Wound edge (margin) can indicate the stage of healing and provide information as to the wound aetiology. The margin type that is good to see is skin that is smooth and adheres firmly to the wound bed.
| TYPE OF MARGIN | INDICATION |
|---|---|
| Maceration | Resulting from prolonged exposure to moisture may occur from incontinence, sweat accumulation, or excess exudate, can cause further breakdown and enlargement of the wound. |
| Desiccation | Removal of physiological fluids that support wound healing, can increase pain and itching. |
| Undermining | Tissue destruction underlying intact skin along the margins can indicate shear. |
| Rolled edges | May indicate wound stagnation or wound chronicity. Dry and with loose skin may indicate additional shearing injury. |
| Steep margins | A punched out appearance often associated with arterial ulceration. |
| Colour | Dusky edges indicate hypoxia; and erythema indicates physiological inflammatory response or cellulitis. |
PERIWOUND SKIN CONDITION
Peri-wound skin condition will provide you with useful information and can alert to problems that can impede healing. The observation of the following should be documented.
Is the surrounding skin:
- Erythematous
- Excoriated
- Desiccated
- Macerated
- Hyperkeratosis
- Callused
- Any skin conditions e.g. eczema
WOUND SYMPTOMS
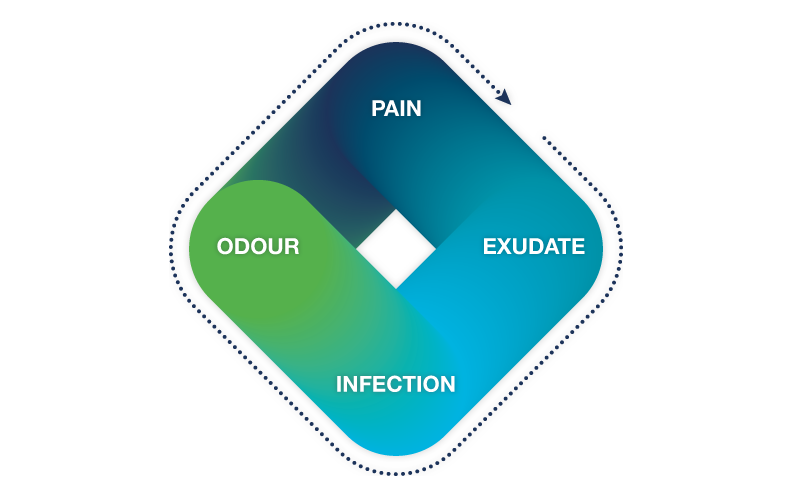
Exudate
Effective management can reduce healing time and related problems. The volume of exudate should reduce as healing progresses. The WUWHS (2007) suggests clinicians should assess and record the following in regards to exudate: colour, consistency, odour and amount. Changes in the volume and type of exudate can provide information on the state of wound healing.
Infection
The wound should be assessed for signs and symptoms of infection. Infection, which include, erythema, swelling, local warmth, heat, pain and also possibly accompanied by a discharge and a pyrexia. The presence of infection will influence the treatment plan and choice of dressing. Systemic infection relating to the wound should be noted, These include; raised temperature, chills, rapid pulse/ breathing and general deterioration.
Specialists
Any referrals to Tissue Viability, Vascular, Podiatry, Dermatology, Plastics or for any other medical opinion, should be included in the assessment along with the referral date. For more information on infection – see our Infection Simplified booklet.
Pain
Wound related pain can change over time and dressing change can be a painful part of wound care.
Careful and ongoing assessment of the levels and type of pain will help to distinguish between pain that is background, provoked by procedures and or due to changing the wound dressings. This allows the relevant pain management to be implemented.
Odour
Wound odour (also referred to as malodour) is usually caused by the breakdown of tissue and typically is a sign of necrosis or infection. A malodorous wound is not directly harmful to a patient but can have a significant psychological impact.
Controlling malodorous wounds will have a positive effect on the patient mental wellbeing and quality of life.
CONCLUSION
Wound assessment is a fundamental aspect of wound management. It is also important to reassess the wound at regular intervals and to change treatment as required. Assessment leads to appropriate treatment aims, and to correct use of a wound care product, which will improve patient outcomes and quality of care.
DOWNLOAD A PDF VERSION OF THIS SIMPLIFIED

